The Important Truth About Postpartum Depression: You Might Not Recognize It Right Away
/*** I had the opportunity to sit down with a fellow mama to chat about her experience battling postpartum depression. For privacy, I’ve changed the names in this post. Here’s her story.***
Jess with her first child, Sarah. Photo courtesy of Jess.
Jess was juggling life as a mother of two young children when she had a sunken feeling of isolation and silence around her postpartum depression (PPD). It was the week Kate Spade and Anthony Bourdain died that prompted her to post her struggles on Facebook. She needed to tell her story.
“All these articles came out about how nobody talks about mental illness and about how a lot of times people don’t reach out. I don’t know if there was anything to prevent it, but I honestly think with postpartum depression there is a lot you can do…if people talk about it,” she told me. Those deaths triggered her to let people know that she wasn’t okay and wanted to talk about it.
Jess and I have known each other for a few years. Our kids went to daycare together and every so often we’d get together for play dates. I had no idea about her struggles until I saw that Facebook post.
As with so many women who experience PPD, Jess’s story is complicated. She didn’t have it with her first child, Sarah, and the signs and symptoms with her second child, Joseph, didn’t appear until close to a year later. What’s more, the symptoms typical of PPD didn’t quite match what she was going through.
Recognizing the Risks for PPD and Preparing for Prevention
Jess has a history of depression and anxiety. She’d been on and off medication for them since she was a teen. In college, she was diagnosed with bipolar disorder and was put on medication but never the right one until 2012. So, when Jess was pregnant with her first child, she was vigilant about self-care and the possibilities of developing PPD.
She explained, “I have an episode every five years or so and it’s usually associated with a transition. I anticipated the struggle. I was terrified I’d have [PPD] with Sarah so I stayed on my medication before and after pregnancy, which is really controversial.”
Jess took a calculated risk and remained on her meds (except one) and continued to work with her therapist. She remembered the birth of her first child, as traumatic. Sarah was premature so she was in the neonatal intensive care unit (NICU) for days. Research has shown mothers with babies in the NICU have higher risk of developing PPD.
At the same time, Jess was losing her mother to ovarian cancer, which increased her worry about developing PPD. But with Sarah, Jess was ecstatic. She never experienced PPD despite her mental health history, grief over her dying mother, and premature newborn.
So, with her second pregnancy Jess thought she was in the clear: “I was like ‘oh, it didn’t happen to me, I beat it, it’s not going to happen,’ which is weird, right, because I was so hyper aware before. After dealing with [mental health] for more than half of my life, I should have been more aware of my triggers, I should have seen this coming, and every single time, I don’t, until I’m in the hole or getting out of it.”
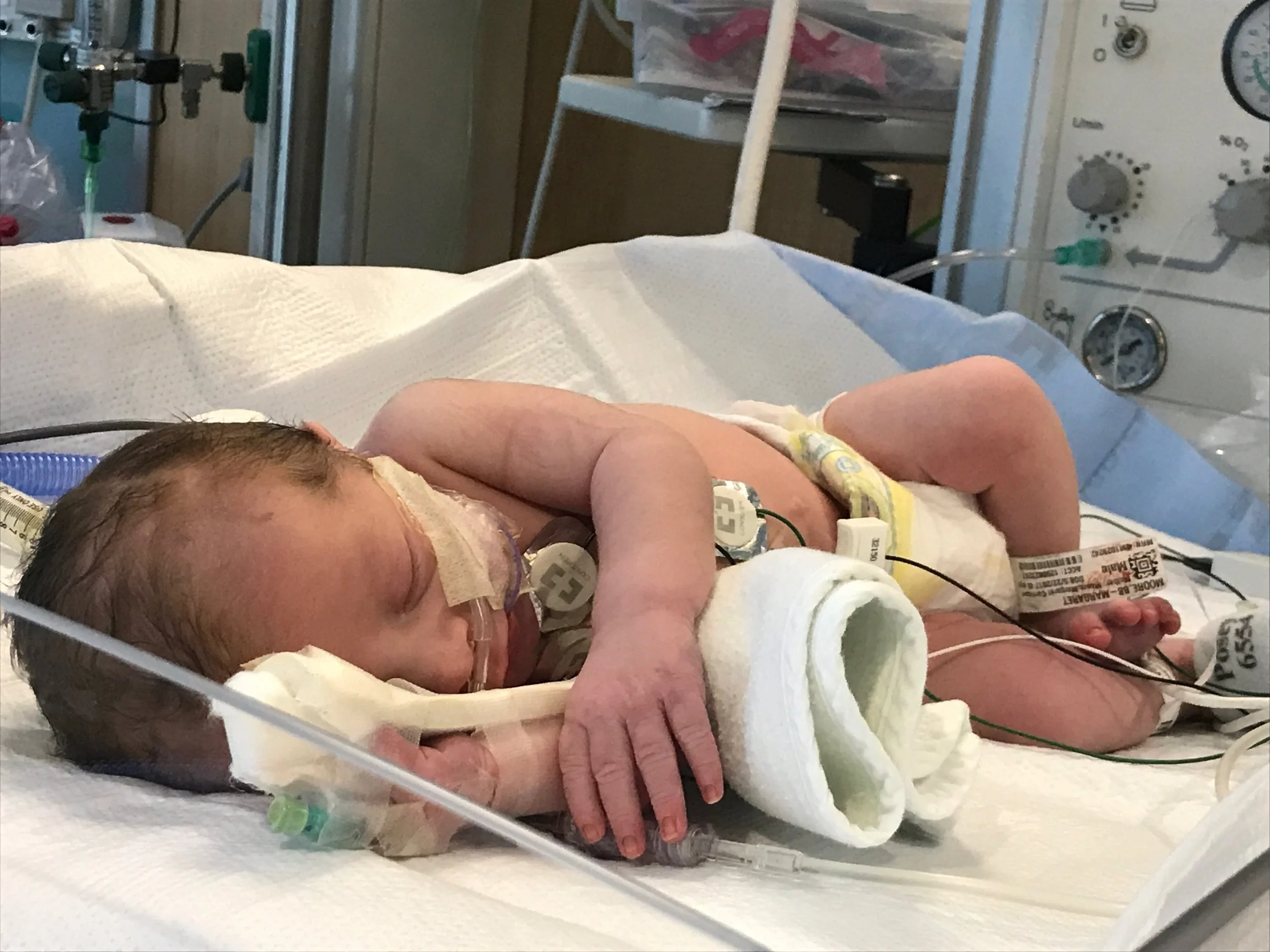
Joseph in the NICU. (Photo courtesy of Jess)
Since Jess thought she “beat” PPD she didn’t prepare for her second child with the same vigilance as her first. Like Sarah, Joseph, also ended up in the NICU (due to breathing problems), but he was only there for 30 hours. Jess was alone at the hospital while her husband took care of Sarah.
During the first half year after giving birth to Joseph, Jess chalked up her irritability to lack of sleep, caring for a toddler and infant, and her son’s round-the-clock nursing.
Jess only realized something wasn’t right until Joseph was closer to a year old. By that time she was struggling to do daily tasks, felt a strain with her husband, and had developed out-of-control anger and rage. Jess told me about this one time, “Joseph wouldn’t sleep, and I was shushing him and I screamed ‘shhh’ and almost shook him and freaked out. [My husband] came in and he was like ‘You need to leave!’ and pushed me away. I drove off into the night in my bathrobe thinking I was going to drive off the road. It was crazy…it escalated into this crazy rage thing where I was screaming at everybody, and it was horrible.”
These behaviors were out of character for Jess. “My whole life I’ve had these episodes of being depressed and my bipolar didn’t express in a typical way. My manic, is taking on the world, working a lot, thinking like I can do everything. My thing is I go up and then I go down and then I’m super anxious, which makes me exhausted. That’s my typical pattern. With Joseph, it wasn’t [like] that. Part of it was losing my mom…and starting to feel really angry. And I never felt angry, really, before in my life. I was always a patient person, kind of a doormat. So this anger was brewing and it didn’t hit until [Joseph] was born,” she told me.
Jess didn’t recognize herself, nor did she recognize her symptoms as PPD because when she read up on it the characteristics didn’t resonate with her. What Jess was experiencing were rapid cycles of mood shifts with rage.
For months she just thought those symptoms were due to sleep deprivation. Joseph was attached to Jess’s breasts day and night. He wouldn’t take a bottle and he wasn’t sleeping through the night in his first year. Jess had accumulated so much sleep debt that even when she had momentary respites with help from her in-laws and a short term night nurse, she never felt rested.
In Hindsight Jess Saw How the PPD Progressed and How She Slipped Through the Cracks
Jess’s first line of action was that she told her therapist about the anger and rage. Her therapist (who wasn’t a psychiatrist) told her to go to the hospital to get a psychiatric assessment and prescriptions for any necessary treatment. Jess was already on medication that helped with her depression and anxiety but resisted anti-psychotics because they posed higher risks to breastfed infants.
That bond Jess felt from breastfeeding Joseph was really important to her. She had already experienced so much loss with her mother’s death. She couldn’t bear anymore loss: “I didn’t want [nursing] to be taken away from me and [with] the medications I felt like that was being taken away from me and I was so pissed. I was like, ‘I’m not [weaning], I’m fine, I just need to get more sleep.’”
Jess researched some of the medications that were prescribed to her. She consulted staff at the Infant Risk Center (IRC) over the phone and they told her the risk levels of certain medications on breastfeeding infants.
Since day one, Joseph wanted to snuggle on mom’s chest, day and night. (Photo courtesy of Jess)
With the guidance of a psychiatrist and information from the IRC, Jess took a measured risk and went on new medication to help manage her mental health. By this time, Joseph was almost a year old so he was taking less breast milk and eating solids.
But the process of getting to the point of seeking help took a huge toll on Jess and her family. Now out of the thick of her struggles, Jess believed that the triggering of her bipolar symptoms and PPD was at Joseph’s birth, or perhaps before.
Despite recognizing it close to a year later, Jess had some vague sense that something wasn’t right early on. “So I remember going to my OBGYN at my six-week checkup and telling [the doctor] I felt out of control. And he didn’t do anything about it. [I was] trying to ask for help, and he did nothing…Maybe he said something but I don’t remember. I remember feeling like he pushed me off and feeling more upset about it. And he’s a good doctor, I just feel like they were trying to check the box,” she explained.
That checkup, for many women, is the only place postpartum moms get screened for PPD, and close to 40% of women don’t even make the visit. Even though Jess went to her six-month postpartum checkup, she somehow fell through the cracks.
The Support to Screen and Intervene on PPD Is Lacking
As Jess reflected on her experience, she grew frustrated with how hard it was to get the support she needed. Even after recognizing she needed help, it took Jess four months to see a dedicated psychiatrist. It was her therapist not her OBGYN who sent her to this hospital’s psychiatric center.
Providers who work with mothers and postpartum women need better training to recognize the nuances of PPD. Jess noticed that her providers never said “they don’t know” or admit to not having answers when she presented issues. Instead, they kept telling her she was just sleep deprived.
Also, the window for catching at-risk moms is small, and the opportunities few. “They assess you at 2-weeks, if you say something maybe 6-weeks. After that, nobody sees you. You don’t have follow up from an OBGYN. You don’t necessarily have help from a lactation consultant unless you’re paying a lot of money. Most people don’t have a therapist because it’s out of reach financially or they don’t think they need it…and most people don’t have access to a psychiatrist,” Jess lamented. With mental health providers, there are also issues of fit, openings for new patients, and affordability. Depending on insurance, your options can be more limited.
When Jess was in the thick of her PPD symptoms, she couldn’t see her situation as she does now. Even though she knew she needed help, that was one more thing to do on her overflowing plate: “Who’s going to say, ‘you need help and I’m going to take you there.’ Because frankly if somebody doesn’t do the research and make the appointment for you, you’re not going to go. If you’re overwhelmed and depressed, how are you going to take that on?”
Jess also wondered about support for her husband. With tears filling her eyes, she told me how her episode with PPD almost destroyed her marriage. Partners aren’t trained to look for or deal with a spouse struggling with mental health issues. “We have breastfeeding classes, we have baby care classes. Why can’t we do emotional support? Your spouse is going to be the one who sees you like that,” she argued.
Although Jess never got to the point of physically harming herself, her children, or getting a divorce, she saw how easily that could have happened. As she gained more distance from her darkest days with PPD and has had a chance to reflect, Jess wanted to share her story with others and to let people know that PPD can happen well after the baby is born, and that it doesn’t look the same for all postpartum women. She has generously allowed me to tell parts of her journey on this blog with hopes of sparking a better conversation about postpartum mental health.
And we are so grateful for her courage.
Have you experienced symptoms of PPD? What kind of help did you receive, if any? How can providers and loved ones better support you?
Resources for PPD
New Mom Checklist for Maternal Mental Health (Below)
**Medical disclaimer: This post is provided as an information resource only. This information should not be used as a substitute for professional diagnosis, treatment, or advice. Always seek the guidance of your physician or other qualified health care provider with any questions you may have regarding your postpartum care and conditions.